Most anesthesia groups still rely on a familiar mix of intuition, block schedules, and contractual coverage targets to staff their operating rooms.
The problem? Those approaches were never designed for today’s environment, where OR demand shifts by the hour, staffing shortages are persistent, and variability is the rule, not the exception.
At the 2026 Anesthesia Economics Summit, Medaxion’s Managing Director of Information Products, Michael Besedick, introduced a different way forward: precision staffing powered by predictive modeling.
It’s a shift away from planning based on assumptions and toward staffing based on what’s actually likely to happen.
The Challenge: Staffing in a World of Constant Variability
There are many ways anesthesia groups attempt to align staffing with OR demand. Most rely on some combination of experience, schedules, and tools. On paper, these approaches seem reasonable. In practice, they consistently fall short.
Some groups lean heavily on institutional knowledge -- years of tradition and experience that help leaders “feel” what coverage is needed. In the best cases, that intuition can be effective. But in many organizations, it breaks down under the weight of provider shortages, turnover, and changing case mix, and ever-evolving organizational priorities.
Others depend on surgical block schedules. These schedules are meant to provide a forward-looking view of OR utilization, but they degrade quickly. Cases shift, add-ons emerge, and variability compounds throughout the day. By the time the schedule is finalized, it’s already outdated.
Workforce scheduling tools, while helpful, often rely too heavily on static schedule inputs and configuration that may have happened years prior. This reinforces preferences or constraints that don’t align with the needs of today, and most platforms do not learn and adapt to what truly happened during the day of surgery.
The result is a pattern most anesthesia leaders know all too well: overstaffing during peak hours and gaps in coverage when demand doesn’t behave as expected.
The Insight: The Schedule Isn’t Reality
When staffing models are evaluated against what actually happens in the OR, the gaps are significant. In one case, we collected data displaying:
-
Schedule-based staffing had an average error rate of ~30%
-
Contract-based staffing performed even worse at ~35%
-
A predictive model reduced that average error to ~15%
This kind of improvement represents a fundamental shift in accurately estimating coverage needs.Ultimately, that accuracy matters to a health system’s bottom line. Every percentage point of error creates pressure on anesthesia operators, budgets, and surgeons that rely on adequate coverage.
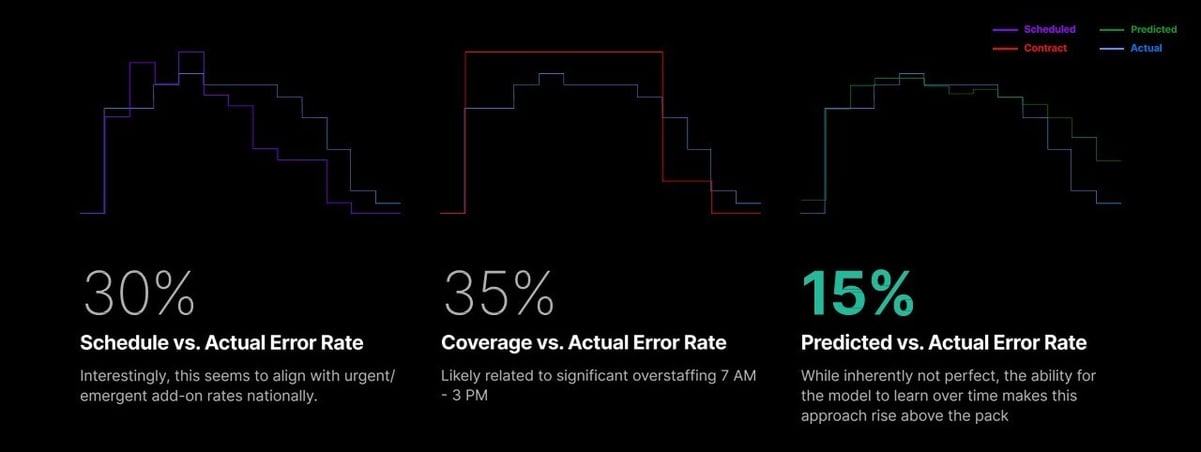
Predictive models cut staffing error rates in half compared to traditional approaches.
The Solution: Precision Staffing
Precision staffing replaces static planning with dynamic modeling.
Instead of asking, “What does the schedule say?” it asks, “What is actually likely to happen?”
Using predicted concurrency (ie “How many rooms are running at each hour of the day?”), this approach incorporates both historical patterns and forward-looking variables. It adjusts for real-world context, including daily variability, seasonality, holidays, and predictably delays and disruptions.
From there, it builds a staffing plan that aligns resources to demand with far greater precision.
The output is the data + insights that Anesthesia Manager is built on. It’s an actionable shift. Leaders can see exactly how to structure their staffing mix across 8-hour, 10-hour, and 12-hour shifts, along with swing and relief coverage, to meet demand as it unfolds.
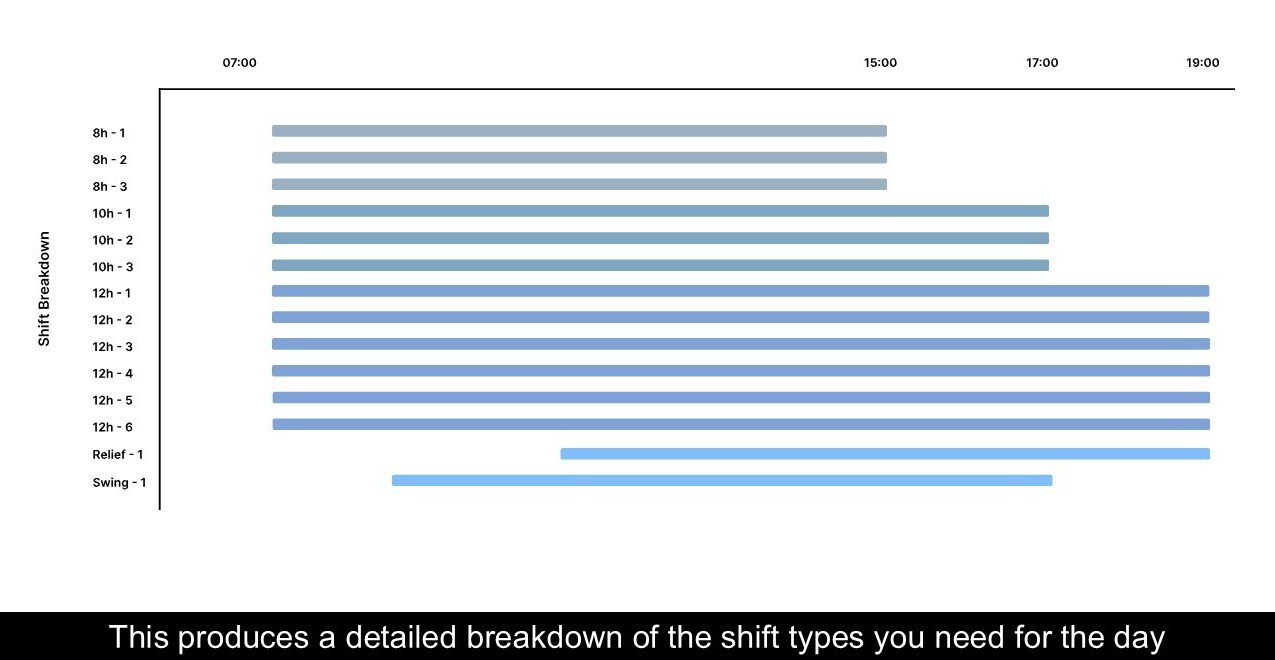
The Impact: Measurable Financial and Operational Gains
For mid-sized facilities that operate between 10 to 15 operating rooms, the impact is both immediate and meaningful.
Organizations implementing this approach have seen annual labor cost reductions in the range of 8–10%, driven largely by better alignment between staffing levels and actual demand.
At the same time, reliance on overtime and locum tenens support decreases, as staffing plans become more intentional and less reactive. Relief and swing shifts are used more effectively, and overall throughput improves.
Perhaps most importantly, the model delivers more than a 2x improvement in coverage prediction accuracy.
That level of precision both improves efficiency and builds confidence. Leaders can make staffing decisions based on data, not guesswork.
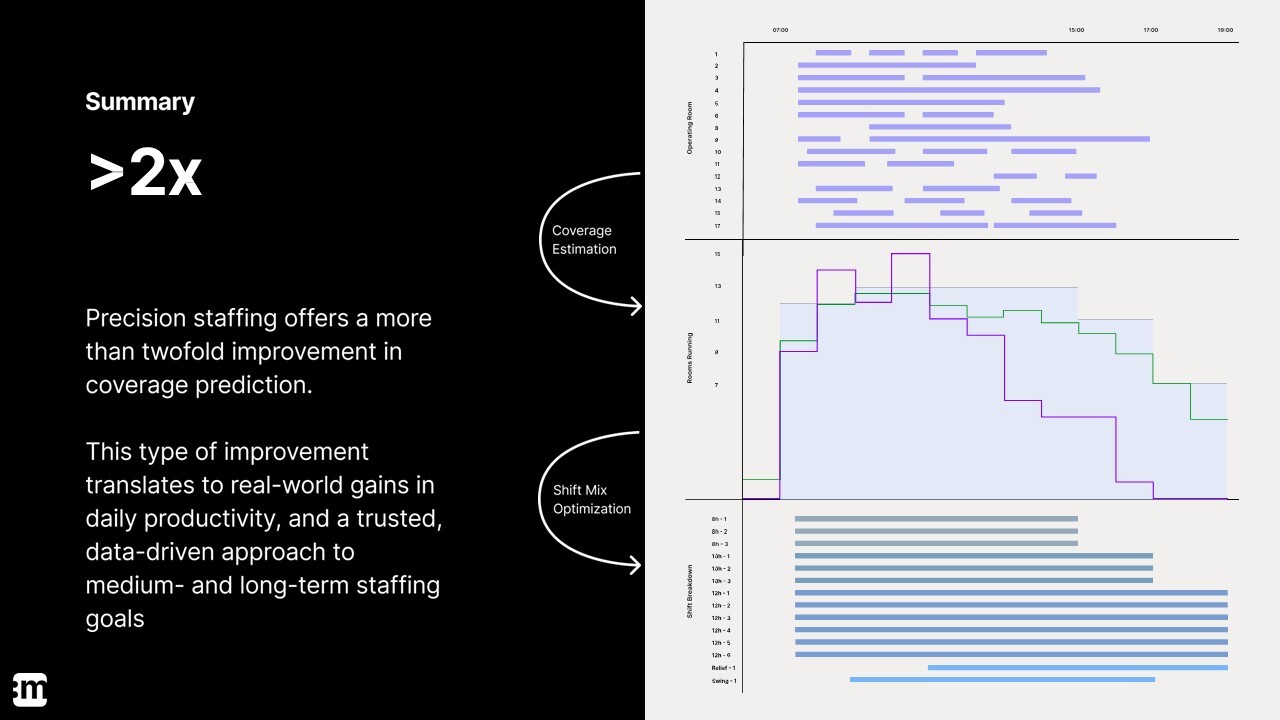
Why It Matters
Anesthesia leaders are facing increasing pressure from every direction. Labor costs continue to rise. Provider shortages persist. Expectations around OR efficiency and throughput have never been higher.
In that environment, traditional staffing models are no longer sufficient.
Precision staffing reframes the problem entirely. It moves organizations away from static plans and toward adaptive, data-driven decision-making.
Because the goal isn’t to staff to what was planned.
It’s to staff to what will actually happen.
See How Your Staffing Model Compares
If your organization is still relying on schedules or contracts to drive staffing decisions, it may be time to take a closer look.
Medaxion’s Anesthesia Manager helps anesthesia leaders model demand, optimize staffing, and align coverage with real-world OR performance.
Request a demo to see how your current model stacks up.